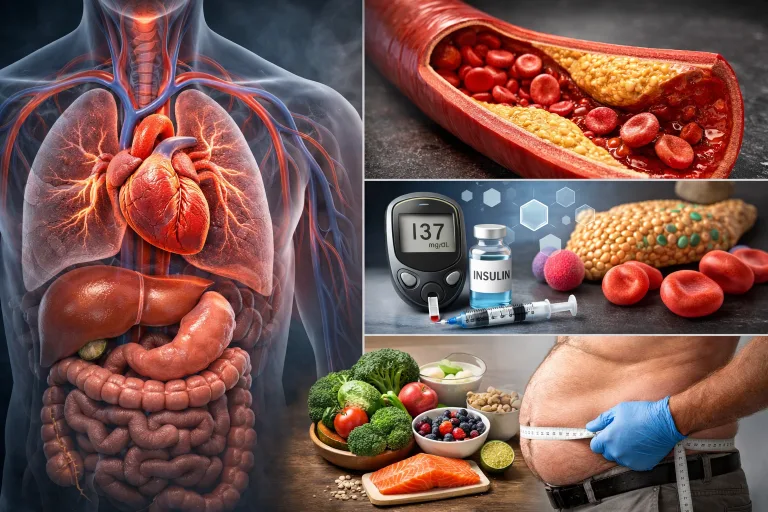
Cardiometabolic health represents an integrated approach to wellness that addresses the interconnected systems governing your heart, metabolism, and increasingly, kidney function. This comprehensive framework—now termed cardiovascular-kidney-metabolic (CKM) health—recognizes that cardiovascular disease, metabolic disorders like diabetes, and chronic kidney disease don’t develop in isolation but through shared pathways involving inflammation, insulin resistance, and dysfunctional fat tissue.[1][2]
The American Heart Association has established a staging system for CKM health ranging from Stage 0 (no risk factors) through Stage 4 (clinical cardiovascular disease), emphasizing that prevention should begin early, often decades before symptoms appear.[1] Maintaining optimal cardiometabolic health reduces your risk not only of heart disease and stroke but also of type 2 diabetes, chronic kidney disease, metabolic-associated fatty liver disease, and even vascular dementia.[3][2]
Recent data reveal a sobering reality: only 6.8% of U.S. adults achieve optimal cardiometabolic health across all five key domains (adiposity, blood glucose, blood lipids, blood pressure, and absence of cardiovascular disease).[3] This underscores both the challenge and the opportunity for preventive intervention.
Traditional cardiovascular risk assessment often focuses on individual risk factors—blood pressure, cholesterol, smoking status—evaluated in relative isolation. Cardiometabolic health takes a fundamentally different approach:
Holistic Integration: Rather than treating high blood pressure, elevated blood sugar, and abnormal cholesterol as separate problems, cardiometabolic health recognizes these as manifestations of underlying metabolic dysfunction, often driven by excess or dysfunctional adipose (fat) tissue.[4][2] For example, visceral fat secretes inflammatory molecules that simultaneously promote insulin resistance, raise blood pressure, and alter lipid metabolism.
Preventive Focus: The CKM staging system identifies risk decades before clinical disease emerges.[1] Stage 1 begins with excess or dysfunctional adiposity, Stage 2 includes metabolic risk factors like hypertension or prediabetes, Stage 3 encompasses subclinical disease, and Stage 4 represents clinical cardiovascular events. This framework enables targeted intervention at each stage.
Comprehensive Risk Assessment: Modern cardiometabolic evaluation extends beyond traditional lipid panels to include inflammatory markers like high-sensitivity C-reactive protein (hsCRP), advanced lipid particles, and markers of insulin resistance.[5][6] The 2025 ACC Scientific Statement now recommends universal hsCRP screening alongside cholesterol measurement.[7]
Integrated Management: Treatment addresses multiple pathways simultaneously. For instance, weight loss through lifestyle modification improves blood pressure, glucose metabolism, lipid profiles, and inflammation concurrently—benefits that exceed the sum of treating each factor individually.[6][8]
The consequences of poor cardiometabolic health extend far beyond a single organ system, see clinical conditions.
Cardiovascular Disease: Metabolic syndrome—defined by the clustering of abdominal obesity, elevated blood pressure, high blood sugar, and abnormal cholesterol—doubles the risk of cardiovascular events and cardiovascular death.[9][10] The risk increases exponentially with each additional metabolic abnormality.[11]
Type 2 Diabetes: Individuals with metabolic syndrome face a 5-fold increased risk of developing diabetes.[12] Conversely, intensive lifestyle intervention can reduce diabetes incidence by approximately 60% compared to placebo.[6]
Chronic Kidney Disease: The CKM framework recognizes that metabolic dysfunction directly damages kidney tissue through inflammation, oxidative stress, and hemodynamic changes.[2]
Cognitive Decline: Cardiovascular and metabolic risk factors contribute to vascular dementia and may accelerate Alzheimer’s disease through impaired cerebral blood flow and chronic inflammation.
Premature Mortality: Poor cardiometabolic health is associated with a 1.5-fold increase in all-cause mortality.[10]
Take a proactive step toward protecting your long-term heart and metabolic health with a personalized functional medicine evaluation that includes advanced cardiometabolic biomarkers, lifestyle assessment, and individualized risk stratification.
Individualized care • Medically supervised • Lab-guided treatment
Comprehensive cardiometabolic assessment requires evaluation across multiple domains:
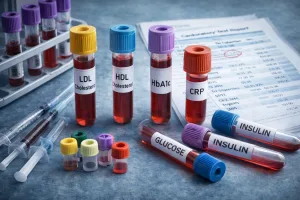
Standard Lipid Panel:
– Total Cholesterol: The sum of all cholesterol in your blood
– LDL-C (Low-Density Lipoprotein Cholesterol): Often called “bad” cholesterol, elevated levels promote arterial plaque formation
– HDL-C (High-Density Lipoprotein Cholesterol): “Good” cholesterol that helps remove excess cholesterol from arteries
– Triglycerides: A type of fat; elevated levels (≥150 mg/dL) increase cardiovascular risk and are a component of metabolic syndrome
Advanced Lipid Markers:
– ApoB (Apolipoprotein B): The primary protein on LDL and other atherogenic particles. Each atherogenic particle contains one ApoB molecule, making this a direct measure of particle number[13][14]
– ApoA1 (Apolipoprotein A-I): The main protein on HDL particles
– ApoB/ApoA1 Ratio: Some evidence suggests this ratio may identify cardiovascular risk earlier than standard lipids, particularly in younger individuals[13][14][15]
Clinical Context: While ApoB and ApoA1 are strong predictors of cardiovascular events, large-scale studies show that when total cholesterol and HDL-C are already measured, adding apolipoproteins provides only minimal additional predictive value for most patients.[16][17] These advanced markers may be most useful in specific situations, such as discordant risk assessments or familial lipid disorders.
– Fasting Glucose: Normal is 100 mg/dL; 100-125 mg/dL indicates prediabetes; ≥126 mg/dL suggests diabetes[3]
– HbA1c (Hemoglobin A1c): Reflects average blood glucose over approximately 3 months. Normal is 5.7%; 5.7-6.4% indicates prediabetes; ≥6.5% suggests diabetes[3]
– Fasting Insulin: Elevated levels may indicate insulin resistance, often present years before blood glucose becomes abnormal
High-Sensitivity C-Reactive Protein (hsCRP): This marker of systemic inflammation has emerged as a clinically actionable biomarker with predictive value comparable to LDL cholesterol and blood pressure.[7][18]
– 1 mg/L: Lower cardiovascular risk
– 1-3 mg/L: Average risk
– >3 mg/L: Higher risk
– >10 mg/L: May indicate acute infection; should be repeated in 2-3 weeks[7]
The 2025 ACC Scientific Statement recommends universal hsCRP screening in both primary and secondary prevention.[7] A 30-year study in women found that hsCRP provided greater risk stratification than LDL cholesterol or lipoprotein(a).[7] Importantly, chronic inflammation is modifiable through lifestyle interventions including weight loss, exercise, smoking cessation, and healthy diet.[7][19]
– Body Mass Index (BMI): Optimal 25 kg/m²; overweight 25-30 kg/m²; obesity ≥30 kg/m²
– Waist Circumference: Reflects visceral (abdominal) fat. Elevated risk: >102 cm (40 inches) in men, >88 cm (35 inches) in women[3]
Important Note: Not all individuals with elevated BMI have poor metabolic health (“metabolically healthy obesity”), and some lean individuals have metabolic dysfunction (“metabolically unhealthy lean”).[6] Waist circumference often better reflects metabolic risk than BMI alone.
– Optimal: 120/80 mmHg without medication
– Elevated: 120-129/80 mmHg
– Hypertension: ≥130/80 mmHg or on blood pressure medication[3]
– ALT (Alanine Aminotransferase): Elevated levels may indicate metabolic-associated fatty liver disease, increasingly recognized as part of the cardiometabolic spectrum[2]
– Creatinine and eGFR (Estimated Glomerular Filtration Rate): Assess kidney function, critical given the kidney’s role in CKM syndrome[1][2]
– Cortisol: The stress hormone influences blood pressure, glucose metabolism, and fat distribution
– TSH (Thyroid-Stimulating Hormone): Thyroid dysfunction affects metabolism, heart rate, and cholesterol levels
– Homocysteine: Elevated levels are associated with increased cardiovascular risk, though routine screening is not currently recommended[5]
Early Detection: Metabolic abnormalities often precede clinical disease by decades. For example, elevated hsCRP can be detected 20 years before cardiovascular events occur.[13] Insulin resistance may develop 10-15 years before diabetes diagnosis.
Personalized Risk Assessment: The combination of multiple biomarkers provides superior risk stratification. Individuals with elevated hsCRP, LDL cholesterol, and lipoprotein(a) experience cardiovascular events several years earlier than those with normal levels.[7]
Treatment Guidance: Biomarker patterns inform therapeutic decisions. For instance, the JUPITER trial demonstrated that individuals with normal LDL cholesterol (130 mg/dL) but elevated hsCRP (≥2 mg/L) experienced a 47% reduction in cardiovascular events with statin therapy.[7][19]
Monitoring Progress: Serial measurements track response to lifestyle and pharmacological interventions, enabling treatment optimization.
The American Heart Association’s “Life’s Essential 8” provides a comprehensive framework for optimizing cardiometabolic health, encompassing diet, physical activity, nicotine exposure, sleep, body weight, blood lipids, blood glucose, and blood pressure.[1][20]
Mediterranean Diet: The most extensively studied dietary pattern for cardiometabolic health, characterized by high intake of vegetables, fruits, whole grains, legumes, nuts, olive oil, and fish, with moderate wine consumption and limited red meat.[6][21][22] This pattern reduces metabolic syndrome risk, inflammation, and hepatic steatosis while improving lipid profiles and insulin sensitivity.
Plant-Based Diets: Emphasizing whole plant foods while minimizing or eliminating animal products improves multiple cardiometabolic risk factors.[21][22]
A proactive, biomarker-driven approach allows these risks to be identified early—often decades earlier—when intervention is most effective. Advanced lipid testing, inflammatory markers such as hsCRP, insulin and glucose dynamics, body composition metrics, and liver and kidney function together provide a far more accurate picture of cardiometabolic risk than traditional screening alone. Importantly, these markers are dynamic and modifiable, meaning targeted lifestyle, nutritional, and medical strategies can meaningfully alter disease trajectory.
At Intercoastal Health, cardiometabolic risk is not addressed in isolation. Instead, it is evaluated within a comprehensive functional medicine framework that seeks to identify root causes, personalize interventions, and monitor progress over time. This approach supports not only disease prevention, but long-term metabolic resilience and healthy aging.
Intercoastal Health provides Testosterone Replacement Therapy (TRT) & Hormone Replacement Therapy , Enclomiphene Citrate Therapy in Jacksonville, FL, delivered through a comprehensive, multimodal approach to healthspan optimization. Our care model integrates evidence-based hormone management with advanced metabolic, lifestyle, and preventive strategies to support long-term vitality and resilience.
In addition, we offer targeted peptide therapies designed to support recovery, tissue repair, and physiological optimization, including BPC-157, Pentadeca Arginate, and Sermorelin—each incorporated into individualized treatment plans based on clinical evaluation and goals.
If you are concerned about insulin resistance, cholesterol abnormalities, inflammation, or weight-related metabolic risk, Intercoastal Health offers integrated services focused on prevention, optimization, and long-term cardiometabolic health.
Individualized care • Medically supervised • Lab-guided treatment




Considering initiating a Cardiometabolic Health Evaluation in Jacksonville, FL? Intercoastal Health offers flexible appointment options, including secure telemedicine consultations, to make comprehensive assessment and care accessible and convenient.
Our clinical team specializes in data-driven cardiometabolic evaluation, utilizing advanced laboratory testing and individualized risk assessment to identify underlying metabolic, cardiovascular, and inflammatory factors. We are available to assist with scheduling your consultation and developing a personalized care plan tailored to your health goals and long-term prevention needs.
Business Hours
Monday: 9AM – 6PM
Tuesday: 9AM – 6PM
Wednesday: 9AM – 6PM
Thursday: 9AM – 6PM
Friday: 9AM – 6PM
Saturday: Closed
Sunday: Closed

Comprehensive care with a whole person approach, specializing in injury management, wellness, and longevity.
3874 San Jose Park Drive
Suite 5
Jacksonville, Florida 32217
Disclaimer: The content on this website is for informational purposes only and does not constitute medical advice or replace professional medical care, diagnosis, or treatment. Eligibility for medical treatments will be determined by your healthcare provider, who will exercise discretion regarding your treatment plan. All images are intended for educational purposes only. Statements made on this website have not been evaluated by the Food and Drug Administration. Always consult your healthcare provider before initiating or discontinuing any treatment.
Intercoastal Health – Copyright © 2026 All Rights Reserved - Privacy Policy